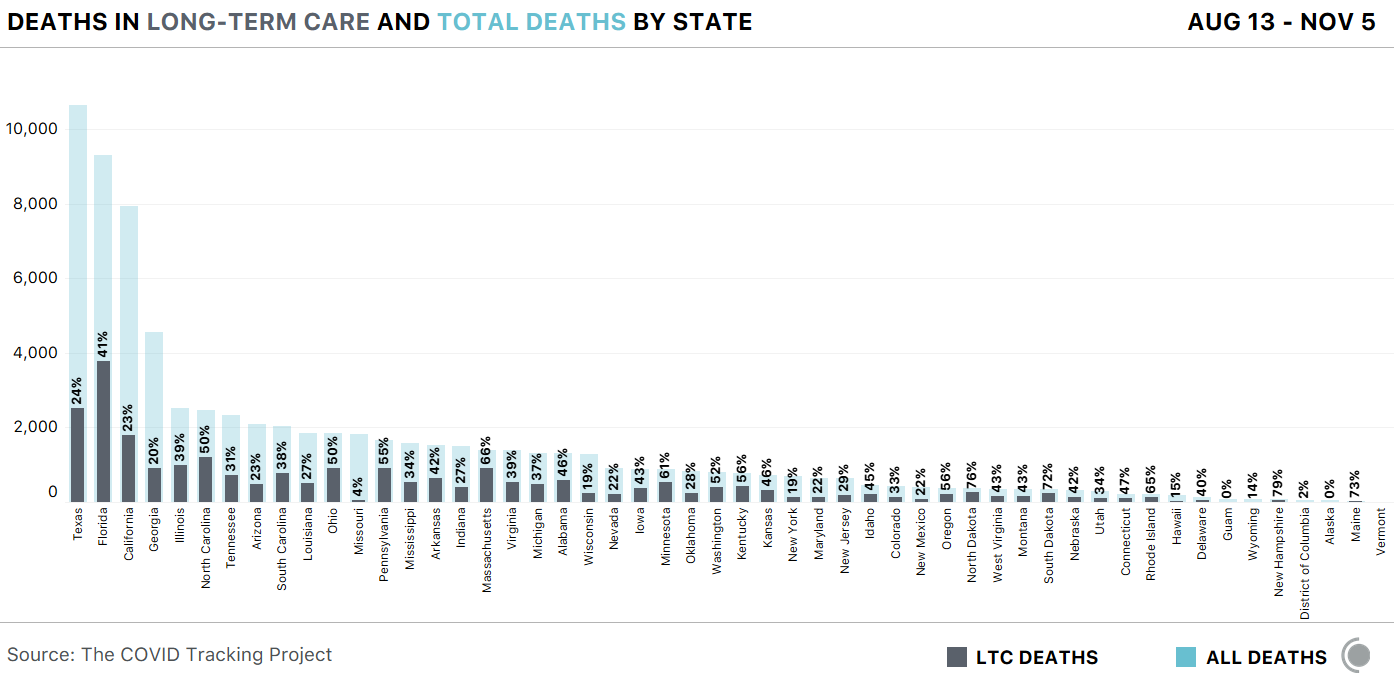
Starting this week, our long-term care team will publish weekly updates on the state of the pandemic in nursing homes, assisted-living facilities, and other long-term care facilities. Since May, we have compiled all the data states provide on cases and deaths within these facilities, where a shocking 40 percent of the nation’s COVID-19 deaths have originated (for more details on our Long-Term Care COVID Tracker, please see our intro post.)
Across the country, COVID-19 is continuing to infect and kill vulnerable residents in long-term care communities. We know that in the beginning of the pandemic, before we were able to collect this data, residents of such facilities were hit particularly hard, but the brutal truth is that eight months and 91,596 long-term-care facility–associated deaths later, cases and deaths are rising once again.
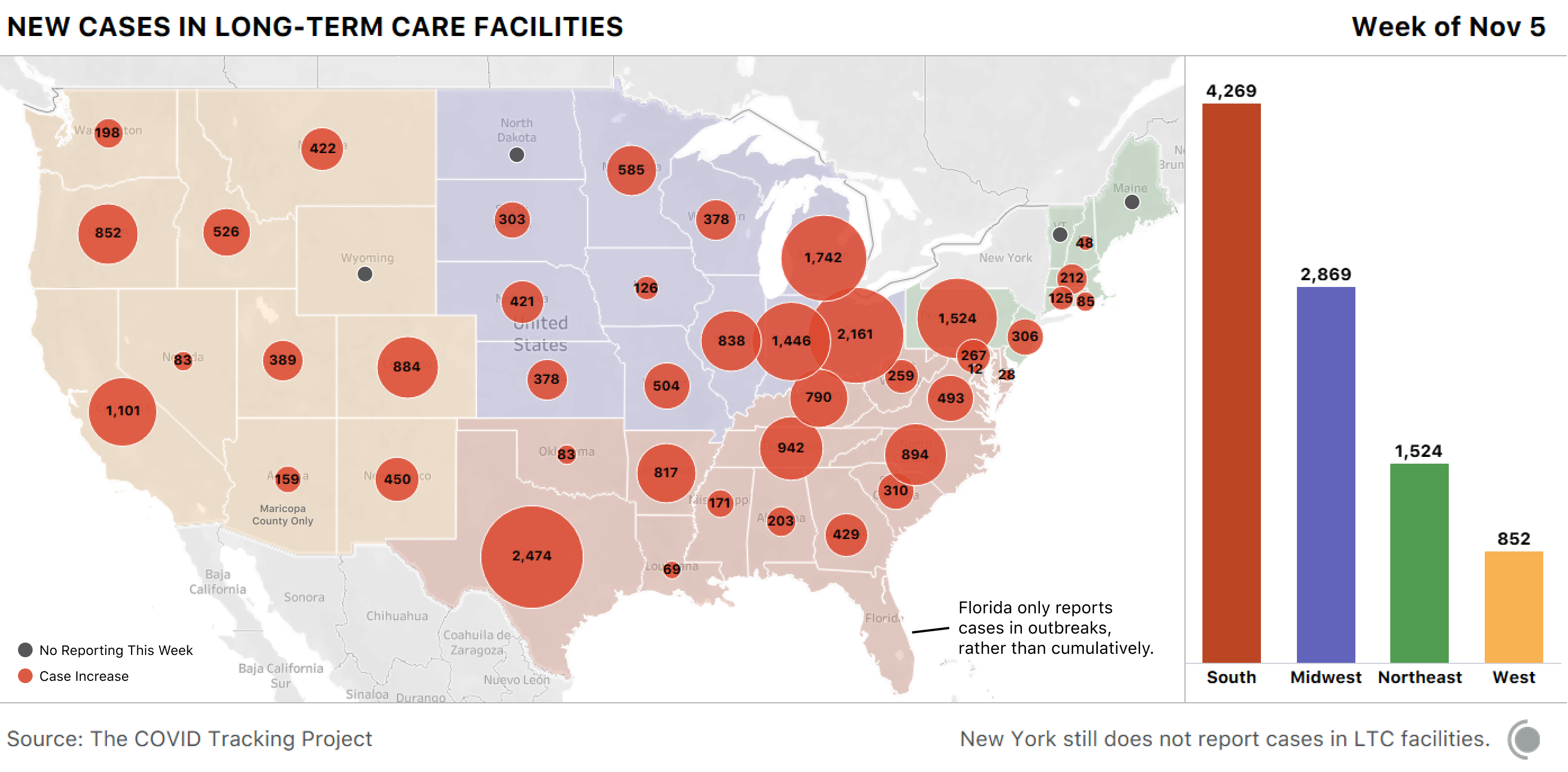
Mirroring the pandemic in the country as a whole, long-term care facilities have seen an alarming rise in cases, with more than 24,000 new cases last week alone. About one-fifth were in three Rust Belt states—Indiana, Ohio, and Pennsylvania. Because a case in a long-term care facility is far more likely to result in death, this explosion in cases is alarming.
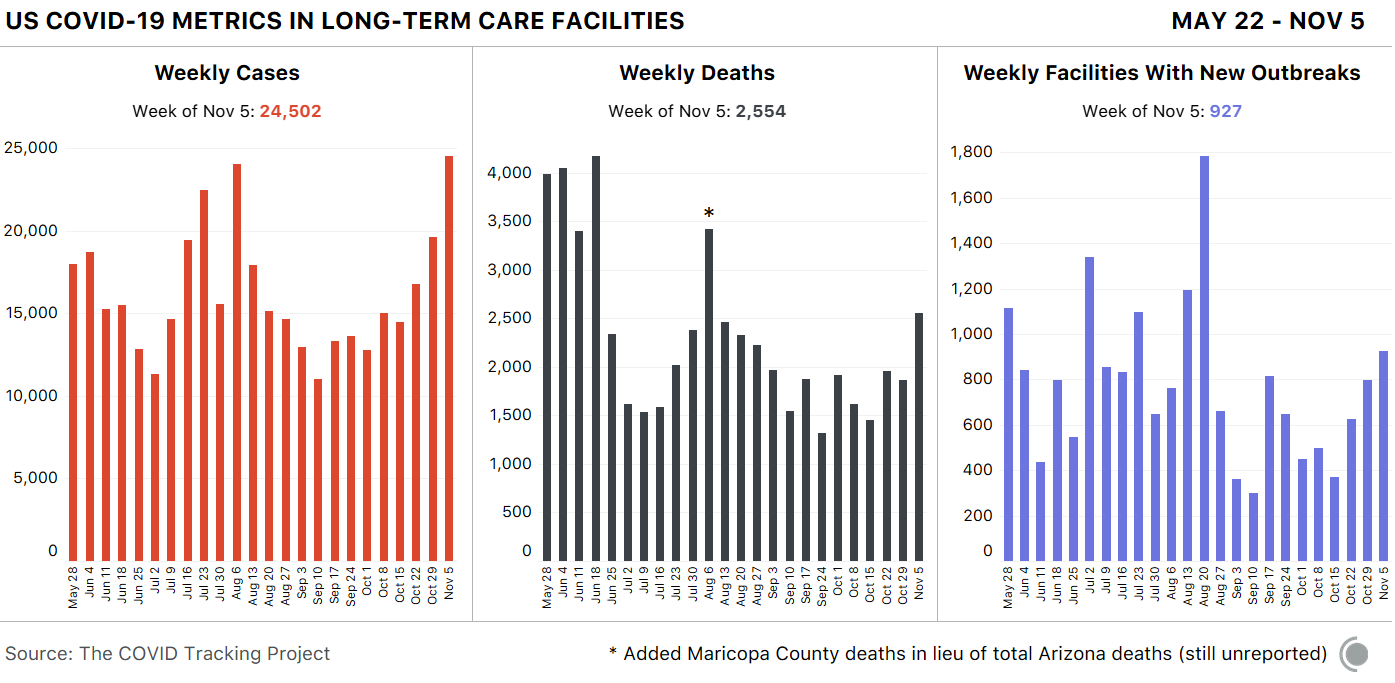
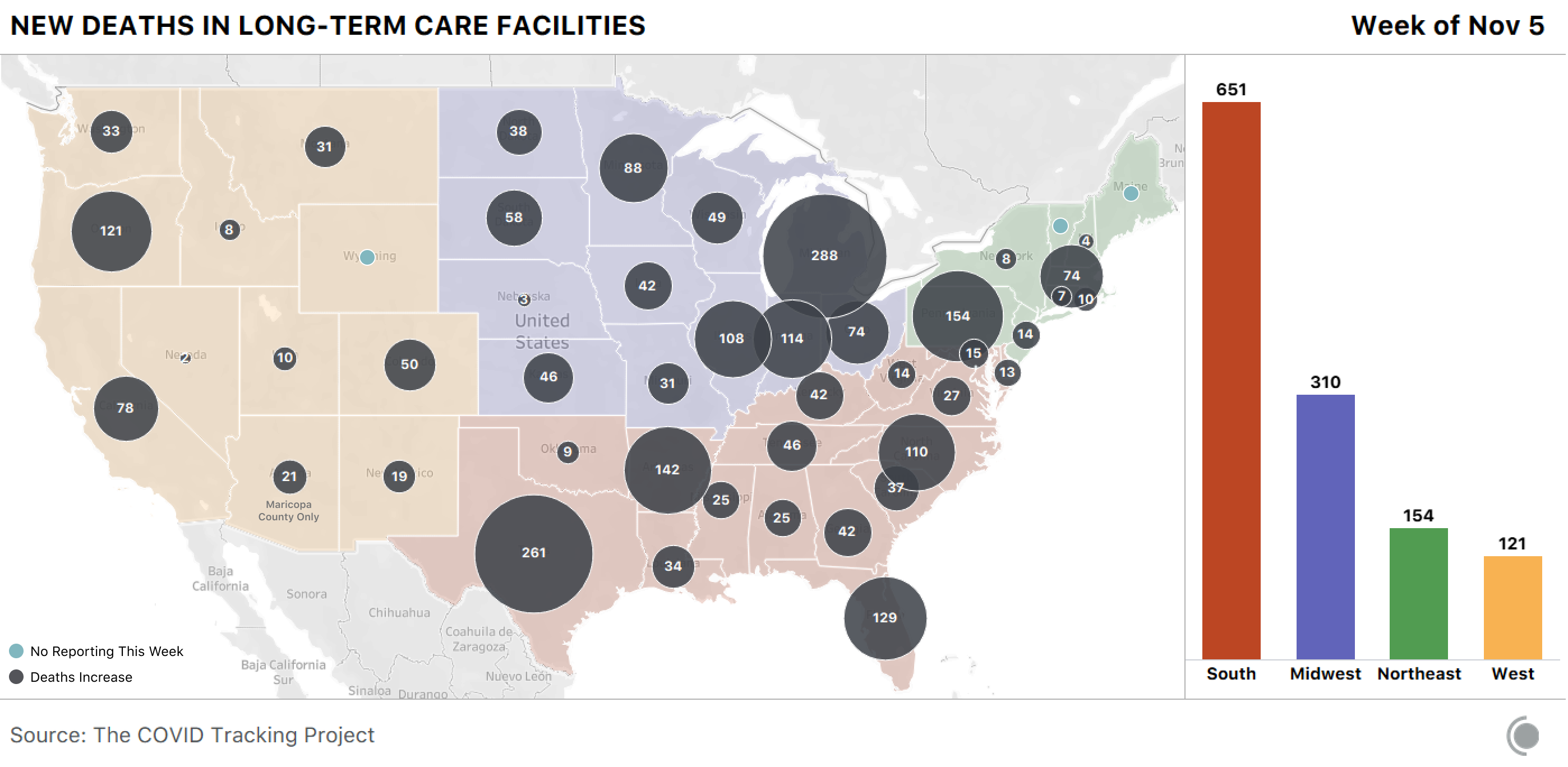
Long-term care deaths are also spiking: 2,554 deaths among residents and staff were reported—an increase of 47.7 percent from the week before. This means that about 383 long-term care staff and residents are dying each day, and the overwhelming majority are residents: In states that report staff and resident deaths separately, 99 percent of the reported deaths are among residents. Four states made up 33 percent of those deaths—Indiana, Ohio, Pennsylvania, and Texas.
Though long-term care facilities accounted for only 4 percent of the nation’s cases from October 29 to November 5, they made up 39 percent of the nation’s deaths during that period.
Case fatality rates in LTCs are down, but still very high
As COVID-19 cases and deaths once again rise in long-term care facilities, we don’t yet know what the impact of this third surge will ultimately be on these vulnerable communities. One spot of hope is that nationwide, fewer people who get COVID-19 are dying when compared to early in the pandemic. But for residents in long-term care facilities, the case fatality rate is still alarmingly high.
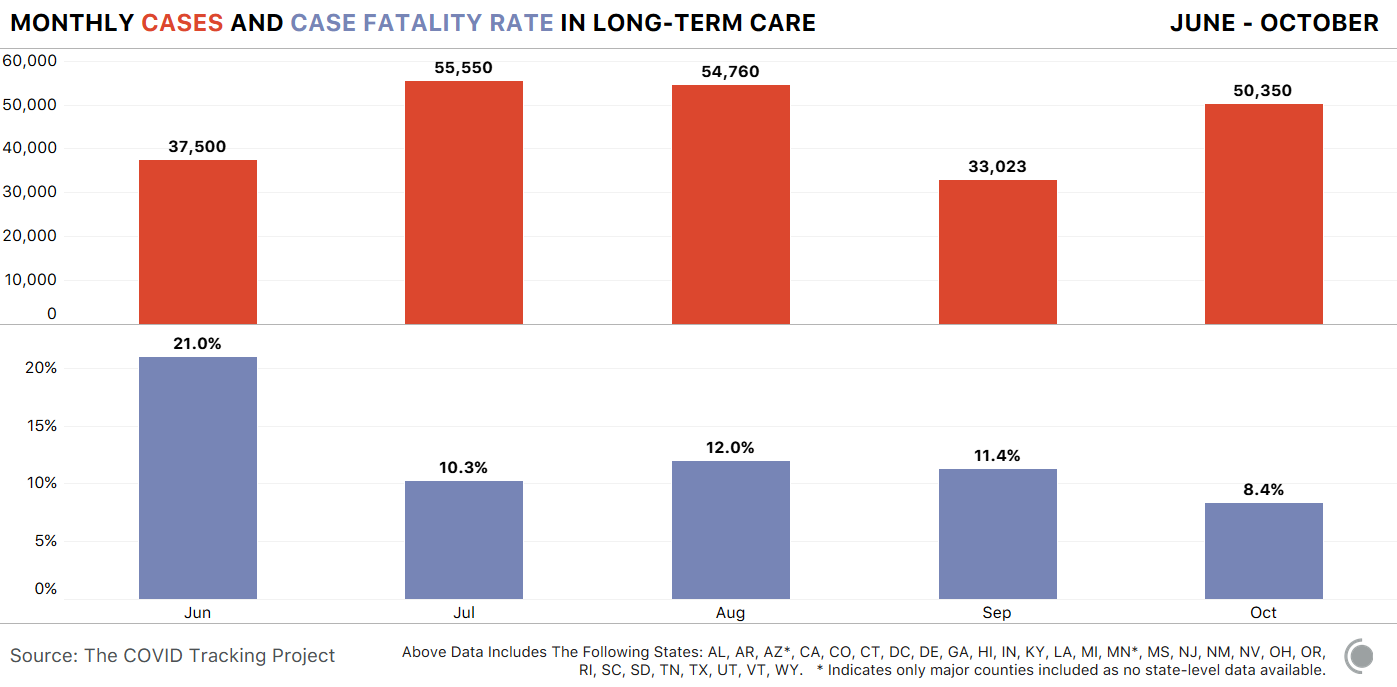
We gather data from every state that provides long-term care data. Of those, 29 states report resident cases and deaths separately from staff cases and deaths. We looked at the case fatality rate (CFR)— a metric for the proportion of confirmed cases that result in a death—to see if more residents are dying from COVID-19 today, as compared to earlier in the pandemic. Based on the data we gathered from states, 8.4 percent of residents with COVID-19 died in October compared with 21 percent of COVID-19 deaths among residents back in June. However, when we compare COVID-19 deaths in long-term care facilities to overall deaths in the United States, the CFR in long-term care facilities is about seven times the national rate in the month of October.
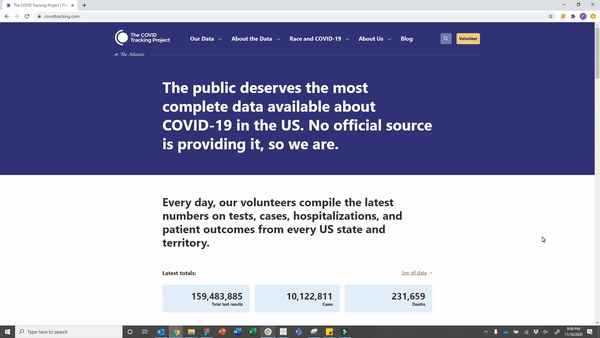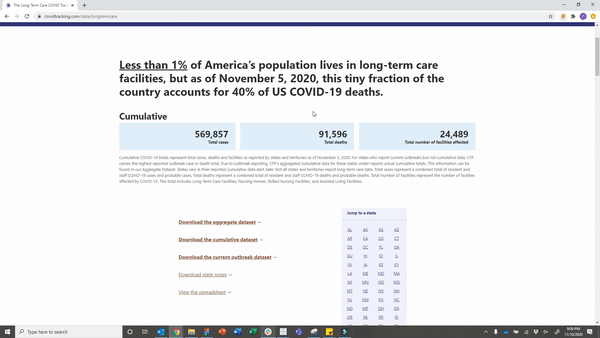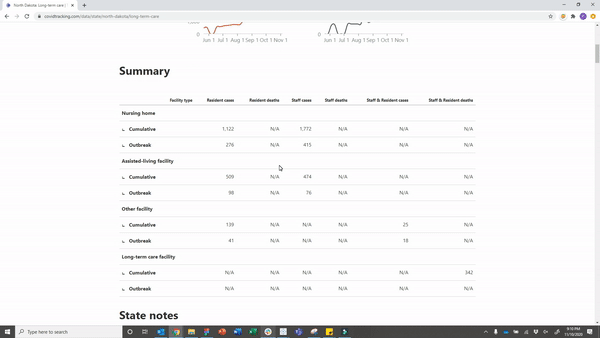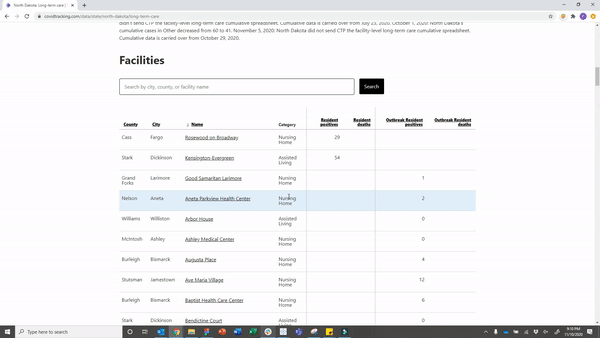
Since August, the Dakotas have been the most dangerous places in the nation for long-term care residents. For the week of October 29 to November 5, 58 of the 79 deaths that occurred in South Dakota were among long-term care residents—73 percent. In North Dakota, 38 of 86 new deaths last week were among long-term care residents and staff—44 percent.
The upshot for this week is this: It may be possible to protect the most vulnerable populations in the United States despite cases and hospitalizations soaring across the country, but so far, we are failing to do so.
Searchable facility-level data is now available
In an effort to shed some light on places where resident cases are spiking, we’ve released new long-term care pages for each US state this week, now including searchable facility-level data. This release provides the most granular look yet available at COVID-19’s effects on residents and staff in US long-term care facilities.
The facility-level information is accessible from our Long-Term Care Tracker main page and from each state’s page in our national dataset. Historic facility-level data is also available to download.

Artis Curiskis is outreach & reporting co-lead at the COVID Tracking Project and collaboratively runs the CTP special projects Long-Term Care COVID Tracker and City Data.

Erin Kissane is a co-founder of the COVID Tracking Project, and the project’s managing editor.

Kara Oehler is outreach & reporting co-lead at the COVID Tracking Project and collaboratively runs the CTP special projects Long-Term Care COVID Tracker and City Data.

Jessica Malaty Rivera has an MS in Emerging Infectious Diseases and is the Science Communication Lead at The COVID Tracking Project.

Aarushi Sahejpal is a Shift Lead on Long-Term Care and City Data at the COVID Tracking Project. She also studies International Relations & Data Science at American University

Sara Simon works on The COVID Tracking Project’s data quality team and is also a contributing writer. She most recently worked as an investigative data reporter at Spotlight PA and software engineer at The New York Times.

Peter Walker is Head of Marketing & Growth at PublicRelay and Data Viz Co-Lead at The COVID Tracking Project.
Nadia Zonis is a New York City-based writer and editor.
More “Long-Term Care” posts
Vaccines Begin to Arrive as Cases and Deaths Keep Rising: This Week in Long-Term Care COVID-19 Data, Dec 16
Cases are up and known deaths in long-term-care facilities are the highest they’ve been since late May.
What We Know—and What We Don’t Know—About the Impact of the Pandemic on Our Most Vulnerable Community
Residents of nursing homes and other long-term-care facilities suffered an outsized impact from COVID-19. And yet we still don’t know how big of an impact, because so much data is missing or incomplete. What we do know makes plain that we failed to protect this community—and at great cost.
Giving Thanks and Looking Ahead: Our Data Collection Work Is Done
While our work to compile COVID-19 data has concluded, we will continue to share research, analysis, and documentation in the months ahead. We are enormously grateful to the hundreds of volunteers who made this work possible.

